Untreated sleep disorders are far more common than most people realize, and public health estimates suggest that around 80% of Obstructive Sleep Apnea cases in the United States remain undiagnosed, which means millions of people struggle every night without a clear explanation for their symptoms. In 2026, timely and accurate sleep disorder diagnosis and testing can protect your heart, brain, mood, and quality of life in very real ways.
Key Takeaways
| Common Question | Concise Answer (2026 Insights) |
|---|---|
| How do I know if I need sleep disorder testing? | If you have loud snoring, pauses in breathing, persistent fatigue, insomnia, unusual movements during sleep, or non-restorative sleep, you should speak with a sleep specialist and consider an evaluation. You can start by locating a clinic near you through resources like the national sleep clinics directory. |
| What is the first step in getting diagnosed? | The process usually begins with a detailed sleep history and physical exam, followed by either an in-lab sleep study or a home sleep apnea test based on your symptoms and risk factors. Guides like the Sleep Foundation overview on finding a sleep doctor can help you prepare. |
| What kinds of tests are used for sleep disorders? | Polysomnography, home sleep apnea testing, actigraphy, and specialty evaluations for narcolepsy and movement disorders are used, depending on what your doctor suspects. Many accredited centers listed in cities like Los Angeles or Orlando provide these services. |
| Are home sleep tests accurate in 2026? | Home sleep apnea tests are reliable for many patients with suspected obstructive sleep apnea, especially when ordered and interpreted by a sleep specialist. Utilization of home testing has grown steadily, and educational resources like Sleep Foundation’s sleep clinic guide explain when they are appropriate. |
| How do doctors decide which sleep test I need? | Clinicians use structured diagnostic algorithms that consider your symptoms, medical history, and risk factors to match you with the right test type. Professional tools such as the American Academy of Sleep Medicine’s diagnostic algorithms, for example the one at SleepEducation.org, guide these decisions behind the scenes. |
| Where can I find an accredited sleep center? | In 2026, there are thousands of accredited centers across the United States, many listed in state and city directories such as Tampa Bay sleep clinics or Atlanta sleep clinics, making it easier to access high quality testing. |
1. Why Sleep Disorder Diagnosis Matters So Much In 2026
In 2026, we recognize that poor sleep is not just an inconvenience, it is closely linked to heart disease, depression, diabetes, accidents, and work impairment. When we diagnose a sleep disorder correctly, we can often improve both nightly rest and long term health risks.
Obstructive Sleep Apnea, insomnia, restless legs syndrome, narcolepsy, and circadian rhythm disorders all require different evaluation paths. Our role is to help you understand which symptoms point to which condition so we can choose the right tests together.


Many patients tell us they delayed testing because they were worried about overnight studies or cost. By walking you through clear diagnostic options, we aim to reduce anxiety and help you feel prepared for each step.
As use of home sleep testing, digital tools, and structured algorithms grows in 2026, getting answers is more accessible than ever if you know where to start.
2. Recognizing Symptoms That Signal You Need Sleep Testing
We recommend formal sleep evaluation when your symptoms are persistent, disruptive, or associated with health changes. You do not need to “prove” your problem first, that is exactly what testing helps clarify.
Common Signs Of Obstructive Sleep Apnea
Obstructive Sleep Apnea is characterized by airflow blockage during sleep, which repeatedly drops oxygen levels and disrupts sleep stages. Symptoms include loud habitual snoring, witnessed apneas or gasping, morning headaches, dry mouth, and daytime sleepiness.
In some people, mood changes, concentration problems, or high blood pressure may be the only noticeable clues. If a partner notices you stop breathing or gasp at night, that alone is a strong reason to seek testing.
Symptoms Suggesting Insomnia Or Circadian Rhythm Problems
Insomnia involves persistent difficulty falling asleep, staying asleep, or waking too early, combined with daytime impairment. Circadian rhythm disorders, like delayed sleep phase, often appear as “night owl” tendencies that clash with work or school schedules.
For these conditions, we may use sleep diaries, questionnaires, and in some cases actigraphy to capture your real world sleep patterns. Your story is central, so we listen carefully before recommending more advanced testing.
When Movement Or Unusual Events Disrupt Sleep
Conditions like periodic limb movement disorder, REM behavior disorder, or parasomnias involve abnormal movements or behaviors during sleep. Bed partners may notice kicking, punching, talking, or sleepwalking.
These issues often require in lab polysomnography with video to capture what happens overnight. Early diagnosis is important in 2026 because some of these conditions can be linked with future neurological illness.
3. The Standard Diagnostic Pathway: From Consultation To Sleep Study
Although each patient is unique, most sleep disorder evaluations follow a similar structure. Understanding this pathway can make the process feel more predictable and less intimidating.
Step 1: Comprehensive Sleep History And Physical Exam
Your first visit focuses on listening to your sleep story in detail. We ask about bedtime routines, sleep timing, awakenings, snoring, medications, mental health, and medical conditions such as hypertension or heart disease.
We may examine your airway, neck, weight, and other physical features that affect breathing. Questionnaires, such as the Epworth Sleepiness Scale, help us quantify your daytime sleepiness and track changes over time.
Step 2: Choosing The Right Diagnostic Test Type
Based on your history and exam, we decide whether you need an in lab study, a home sleep apnea test, or a different type of evaluation. Behind the scenes, clinicians increasingly rely on structured decision tools like the diagnostic algorithms published by the American Academy of Sleep Medicine, for example those described at SleepEducation.org.
For straightforward suspected Obstructive Sleep Apnea without major heart or lung disease, a home sleep apnea test is often appropriate. For more complex symptoms, or when we suspect multiple disorders, we usually recommend a full in lab polysomnogram.


Step 3: Explaining Results And Building A Treatment Plan
After your test, we review both the numbers and what they mean for your daily life. We explain your apnea hypopnea index, oxygen levels, arousals, sleep stages, and any movements or unusual behaviors we recorded.
Our goal is to connect these findings with specific treatment recommendations, such as CPAP, oral appliances, positional therapy, behavioral treatment for insomnia, medication, or light therapy for circadian disorders.
A visual guide to the five essential steps in diagnosing and testing sleep disorders. It highlights what clinicians evaluate and why each step matters.
4. In-Lab Polysomnography: What To Expect During An Overnight Sleep Study
Polysomnography is the gold standard overnight test for many sleep disorders. In 2026, labs focus on comfort, privacy, and clear explanations to help you rest despite the unfamiliar environment.
How An Overnight Study Is Set Up
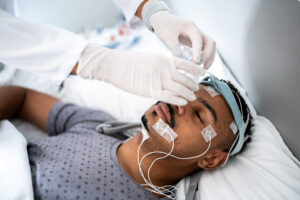
When you arrive, a technologist places small sensors on your scalp, face, chest, and legs to measure brain waves, eye movements, muscle tone, heart rate, breathing, oxygen levels, and limb movements. The setup is painless, and the wires are long enough to allow you to change position normally in bed.
A video camera records your sleep so we can correlate movements or behaviors with changes in your brain and breathing signals. Throughout the night, staff monitor your signals from a control room and can assist you if you wake or need the restroom.


Split-Night And Titration Studies For Sleep Apnea
If you clearly show Obstructive Sleep Apnea early in the night, we may convert to a split night study, in which we start CPAP mid-study to find the right pressure in one visit. For known sleep apnea, a separate titration study fine tunes your CPAP settings to prevent events while keeping you comfortable.
In 2026, some labs also evaluate alternative therapies like bilevel PAP or adaptive servo ventilation when central apnea or hypoventilation is present. The technologist adjusts equipment in real time based on your data as you sleep.
Who Benefits Most From In-Lab Studies
We generally recommend in-lab polysomnography if you have heart failure, lung disease, neuromuscular illness, suspected narcolepsy, parasomnias, or periodic limb movement disorder. Children and older adults with complex symptoms also often benefit from the extra monitoring and safety of a lab environment.
You are not expected to sleep perfectly, and even a few hours of monitored sleep can provide enough information for diagnosis. Our team’s job is to make the night as smooth as possible, answer your questions, and ensure you feel supported throughout.
5. Home Sleep Apnea Testing (HSAT): Convenient Diagnosis From Your Bed
Home Sleep Apnea Testing has grown dramatically, and in 2026 it is a central option for many adults with suspected Obstructive Sleep Apnea. These tests measure breathing, oxygen, and heart rate while you sleep at home using a small portable device.
Who Is A Good Candidate For HSAT
We consider HSAT if you have symptoms strongly suggesting obstructive sleep apnea and no major complicating conditions such as severe lung disease, neuromuscular disorders, or opioid use. For these straightforward cases, HSAT can accurately confirm moderate to severe sleep apnea.
If your HSAT is inconclusive or negative yet symptoms persist, we often follow up with a full in lab study. This stepwise approach keeps your care efficient while avoiding missed diagnoses.
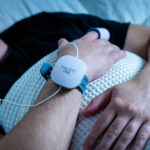
How HSAT Devices Work In 2026
Modern home testing units are smaller and more user friendly than earlier generations. Most systems include a nasal cannula or sensor to measure airflow, a belt to track breathing effort, and a finger probe for oxygen saturation and pulse.
We show you how to apply the sensors and start the recording before you take the device home. The next day, you return the equipment, and a sleep specialist interprets the data within a few days.

Understanding The Limits Of Single-Night Home Tests
Research shows that sleep apnea severity can vary significantly from night to night, and nearly 70% of patients in some studies showed important variation across multiple HSAT nights. This means a single normal test does not always rule out a problem if your symptoms are strong.
In 2026, more clinicians consider multi night home testing strategies or repeat studies when clinical suspicion remains high. We discuss these options openly with you so that negative results are interpreted carefully, not as the end of the story.
6. Specialized Testing For Insomnia, Narcolepsy, And Movement Disorders
Not all sleep disorders are driven by breathing issues, and in 2026 we have more targeted tests for other conditions. These specialized evaluations often combine objective measurements with structured interviews and behavioral assessments.
Insomnia Evaluation: When Do We Test Beyond The Interview
For chronic insomnia, the foundation of diagnosis is your sleep history, daytime functioning, and mental health context. We may ask you to keep a sleep diary or wear an actigraphy watch that tracks movement and light exposure to understand your patterns over weeks.
In some cases, we perform polysomnography to rule out coexisting disorders like sleep apnea or periodic limb movements that can aggravate insomnia. Treatment then focuses on cognitive behavioral therapy for insomnia, medication in certain scenarios, and lifestyle adjustments.
Testing For Narcolepsy And Hypersomnia
When excessive daytime sleepiness is severe, we evaluate for narcolepsy or idiopathic hypersomnia. The Multiple Sleep Latency Test (MSLT) follows an overnight polysomnogram and measures how quickly you fall asleep during short daytime nap opportunities.
We also look for REM sleep occurring too early during these naps, which is characteristic of narcolepsy. This careful protocol ensures we base long term diagnoses on solid objective evidence.


Evaluating Restless Legs Syndrome And Periodic Limb Movement Disorder
Restless Legs Syndrome is diagnosed mainly from your description of an uncomfortable urge to move the legs at night, which improves with movement and worsens at rest. Polysomnography can quantify periodic limb movements that occur during sleep and disturb your rest.
Blood work sometimes checks for iron deficiency and other contributing factors. By combining these data with your symptoms, we personalize medical treatment and lifestyle strategies that reduce both leg discomfort and sleep disruption.
7. How To Find Accredited Sleep Clinics And Centers Near You
In 2026, one of the most practical questions we hear is simply, “Where should I go for testing?” Choosing an accredited center with experienced clinicians is as important as choosing the test type itself.
Using National And City-Level Directories
Online directories list accredited sleep clinics by state and city, including how many centers operate in each area and which specialize in pediatric versus adult care. For example, if you live in Alabama you can review providers in Birmingham or Montgomery to compare options.
Residents in larger metropolitan areas benefit from multiple centers, such as the 34 clinics listed for Los Angeles, California, while smaller cities like Rome, Georgia also maintain dedicated sleep medicine resources.
Regional Examples: Georgia And Florida
If you are based in Georgia, directories list dozens of clinics, including those in Atlanta where around 47 centers are cataloged, to ensure urban and suburban patients have access. Smaller communities, such as those served by the clinics around Rome, allow patients to stay closer to home while still receiving competent testing.
Florida residents can explore listings in Orlando, Tampa Bay, or Gainesville, where pediatric centers, adult centers, and multi specialty practices all provide diagnostic studies. These directories save time and help you focus quickly on accredited, nearby facilities.


Checking Accreditation And Scope Of Services
When you review a clinic, we encourage you to look for accreditation by recognized bodies such as the American Academy of Sleep Medicine. This signal means the center meets standards for staffing, equipment, and safety.
You should also confirm whether the clinic performs adult, pediatric, or both types of studies, what kinds of tests they offer, and whether they provide follow up treatment in-house. A center that integrates diagnosis and long term management can simplify your journey from testing to therapy.
8. Preparing For Your Sleep Test: Practical 2026 Checklist
Good preparation helps you get the most accurate results from your sleep study, whether it is at home or in the lab. We provide clear, written instructions before your test and answer any questions you may have.
Day-Of-Study Guidelines
On the day of your overnight study, we usually recommend avoiding naps and limiting caffeine, especially late in the day. You should take your regular medications unless we specifically advise changes, and bring a full list of your prescriptions and supplements.
For in-lab polysomnography, we ask you to bring comfortable sleepwear, toiletries, and any items that make you feel at home, such as your pillow. Eating a light evening meal and arriving on time help the evening unfold smoothly.
What To Bring To An In-Lab Study
- Photo ID and insurance information.
- Comfortable pajamas and a change of clothes for the morning.
- All medications you normally take at night or early morning.
- Reading material or a quiet activity while we place your sensors.
For home tests, you take the small recording device and instructions home with you. We show you how to apply the sensors and ask you to follow your typical bedtime routine as closely as possible.


Managing Anxiety About The Test
Feeling nervous is very common, especially before your first sleep study. We encourage you to share any specific worries, such as claustrophobia, mobility limitations, or concerns about CPAP masks, so we can plan accommodations ahead of time.
Remember that your role is simply to try to sleep as you normally would, not to perform. Our staff has guided thousands of patients through this process, and we remain close by throughout the night to support you.
9. Understanding Your Results And Next Steps After Diagnosis
After testing, we schedule a dedicated follow up visit to go through your results in plain language. We want you to leave that appointment knowing exactly what we found and what we recommend next.
Key Metrics In Sleep Apnea Reports
Your report for Obstructive Sleep Apnea will highlight the Apnea Hypopnea Index (AHI), oxygen desaturation levels, sleep stages, and arousal index. We categorize OSA severity as mild, moderate, or severe based on the AHI and match treatment intensity to this level.
We also discuss positional patterns, such as apnea worsening when you sleep on your back, which can inform non device strategies like positional therapy. If REM sleep makes events worse, that finding may guide medication choices and counseling.
Linking Diagnosis To Personalized Treatment
Diagnosis is only useful if it leads to an actionable plan, so we spend time reviewing every option that fits your situation. That may include CPAP, oral appliance therapy, weight management, surgery for selected cases, or behavioral treatments for insomnia.
For complex disorders, we may involve neurology, psychiatry, cardiology, or pulmonary specialists to build a coordinated plan. Our goal is to align the science of your test results with your personal goals and preferences so that your treatment is realistic and sustainable.


Planning Follow Up And Monitoring
In 2026, follow up is an integral part of sleep medicine, especially for CPAP users and patients with progressive conditions. We schedule visits to check your adherence, comfort, symptom relief, and any side effects of treatment.
We may also repeat testing after significant weight changes, surgery, or if symptoms recur. The objective data from your devices and studies help us keep your care optimized over the long term.
10. The Future Of Sleep Disorder Testing: 2026 And Beyond
Sleep medicine is evolving quickly, and diagnosis in 2026 already looks different from a decade ago, especially in how we use home testing and digital tools. These innovations aim to make testing more accessible without sacrificing accuracy.
Growth Of Home-Based And Digital Diagnostics
Utilization data show that home sleep apnea testing has expanded substantially over the past decade, and in some insurance populations it now accounts for a large share of initial diagnostic tests. This trend is likely to continue as device accuracy improves and telehealth workflows mature.
We increasingly combine HSAT data with wearable information, symptom questionnaires, and telemedicine visits to monitor sleep health over time. This continuous view can catch changes earlier than occasional in lab testing alone.
Role Of AI And Advanced Analytics
Artificial intelligence is beginning to assist with automated scoring of sleep studies and prediction of disease risk. Research models already achieve high accuracy in classifying apnea and other events across diverse datasets, suggesting that clinical tools may soon offer faster, more standardized interpretations.
Our responsibility as clinicians in 2026 is to use these technologies as decision support, not replacements for clinical judgment or patient centered discussions. We remain accountable for explaining your results and recommendations clearly, regardless of how the data are processed.
Adapting Testing Pathways For An Aging Population
As the US population ages, Obstructive Sleep Apnea and other sleep disorders in older adults are projected to rise sharply by 2050. This demographic shift means more patients with multiple medical conditions, mobility limitations, and caregiving responsibilities will need tailored diagnostic approaches.
We expect further growth in home-based testing, more flexible lab environments, and closer partnership with primary care and geriatric services. Throughout these changes, our focus remains the same, providing clear, compassionate, and evidence based guidance so that every patient, at any age, can pursue better sleep and better health.
Conclusion
Sleep Disorder Diagnosis and Testing in 2026 brings together advanced technology, large networks of accredited clinics, and structured clinical pathways to give you clear answers about your sleep. Whether you undergo an in-lab polysomnogram, a home sleep apnea test, or specialized evaluations for insomnia or narcolepsy, the goal is always the same, to understand what is happening at night so we can improve how you feel during the day.
If your sleep leaves you exhausted, foggy, or worried, you do not need to navigate this alone. Reaching out for evaluation is a decisive first step, and with the tools available today, we can work with you to identify the problem, explain your options, and support you through treatment that helps you reclaim more restful nights and healthier days.
========================================